Are nurses allowed to give injections?
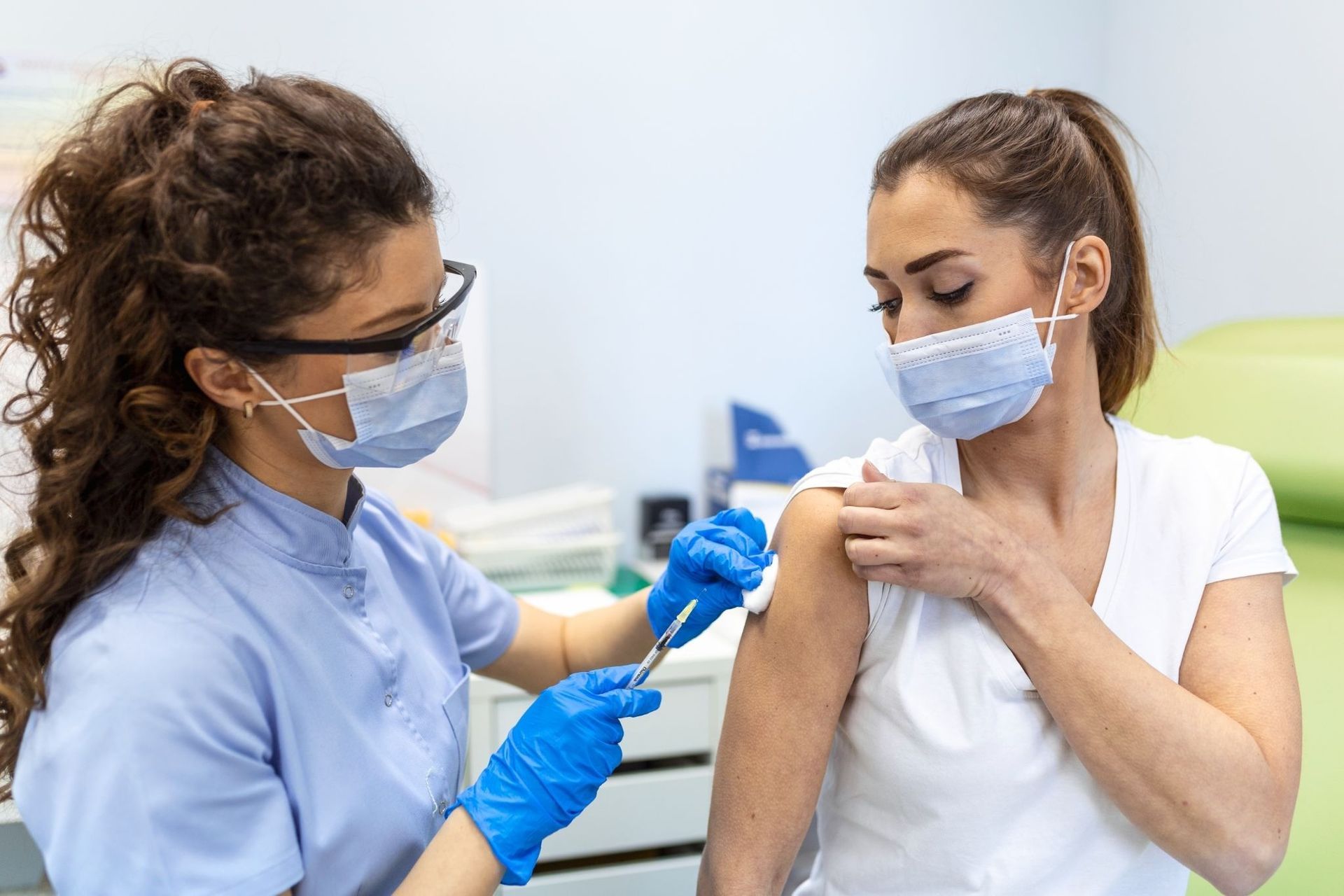
In healthcare settings across the United Kingdom, injections are a routine yet critical part of patient care. From administering vaccines to delivering life-saving medications, injections require precision, training, and professional accountability. A common question often raised by patients, carers, and even those considering a career in healthcare is: are nurses allowed to give injections?
The short answer is yes. However, the full picture involves regulation, training, competence, and scope of practice. This article explores the legal framework, professional standards, and practical responsibilities surrounding nurses and injections, helping you understand not just whether nurses can administer injections, but how and why they do so safely.
Understanding the Role of Nurses in Clinical Practice
Nurses play a central role in modern healthcare. Their responsibilities extend far beyond basic care, encompassing clinical procedures, patient education, medication administration, and ongoing monitoring. Administering injections is one of the many tasks nurses perform as part of their everyday duties.
In the UK, nurses are regulated by the Nursing and Midwifery Council (NMC). The NMC sets the standards for education, training, and professional conduct. Any nurse registered with the NMC is expected to practise safely, effectively, and within the limits of their competence.
Administering injections falls well within the scope of nursing practice, provided the nurse has received appropriate training and is deemed competent.
What Types of Injections Can Nurses Give?
Nurses in the UK are trained to administer a wide range of injections. These include:
Intramuscular Injections
These are delivered into the muscle, commonly in the upper arm, thigh, or buttock. Vaccines such as flu jabs and certain medications are often given this way.
Subcutaneous Injections
These are administered just beneath the skin. Insulin for diabetes and some anticoagulant medications are typical examples.
Intradermal Injections
Given into the top layer of the skin, these are often used for allergy testing or tuberculosis screening.
Intravenous Injections
Some nurses, particularly those in hospital settings or with specialist training, can administer injections directly into a vein. This requires a higher level of competence and is usually performed by experienced or specially trained nurses.
Each type of injection requires a specific technique, understanding of anatomy, and awareness of potential risks.
Legal Framework Governing Nurses and Injections
The administration of injections by nurses is governed by UK law and professional guidelines. Nurses must follow:
- The NMC Code, which outlines standards of practice and behaviour
- Medicines management policies set by their employer
- National guidelines such as those from the National Institute for Health and Care Excellence (NICE)
Nurses are legally permitted to administer injections under several frameworks:
Patient Specific Directions
A doctor or prescriber may issue a prescription for a named patient. The nurse administers the injection according to those instructions.
Patient Group Directions
These allow nurses to supply and administer medicines to groups of patients without a prescription. This is common in vaccination programmes.
Independent Prescribing
Some nurses are qualified as independent prescribers. This means they can prescribe and administer medications, including injections, without needing approval from a doctor.
Each of these frameworks ensures that patient safety remains the priority.
Training and Competence
Before a nurse is allowed to give injections, they must undergo comprehensive training. This begins during their nursing education and continues throughout their career.
Training covers:
- Anatomy and physiology
- Pharmacology
- Injection techniques
- Infection prevention and control
- Safe handling and disposal of sharps
Competence is not a one-time achievement. Nurses are expected to maintain their skills through continuous professional development. Employers often require regular assessments to ensure that nurses remain competent in administering injections.
Safety Considerations
Administering injections carries risks, including infection, allergic reactions, and incorrect dosage. Nurses are trained to minimise these risks through strict safety protocols.
Key safety measures include:
- Verifying the correct patient, medication, dose, route, and time
- Using sterile equipment
- Following proper hand hygiene
- Disposing of needles safely in sharps containers
- Monitoring patients for adverse reactions
Patient consent is also essential. Nurses must explain the procedure, address concerns, and obtain informed consent before proceeding.
Can All Nurses Give Injections?
While most registered nurses are trained to give injections, not all nurses perform this task regularly. The ability to administer injections depends on:
- The nurse’s role and work setting
- Their level of training and experience
- Employer policies and protocols
For example, a community nurse, practice nurse, or hospital nurse is likely to administer injections frequently. In contrast, a nurse working in a non-clinical role may not.
The key principle is that nurses must only perform tasks they are competent to do.
The Role of Specialist Nurses
Certain nurses undergo additional training to specialise in areas where injections are a core part of care. These include:
- Diabetes nurses who manage insulin therapy
- Immunisation nurses who run vaccination clinics
- Oncology nurses who administer chemotherapy
- Aesthetic nurses who provide cosmetic injections
Specialist training ensures that these nurses have advanced knowledge and skills tailored to their field.
Injections in Community and Home Care Settings
In recent years, there has been a growing demand for healthcare services delivered at home. Nurses working in community settings often administer injections to patients who cannot attend clinics or hospitals.
This includes:
- Elderly patients requiring regular medication
- Individuals with chronic conditions
- Post-operative patients needing pain relief or antibiotics
Home-based care offers convenience and comfort for patients while maintaining high standards of clinical care.
For those seeking professional and reliable
nursing services at home, platforms such as
Nurse Agnes provide access to qualified nurses who can safely administer injections and other treatments in a familiar environment.
Common Misconceptions
Despite clear regulations and widespread practice, there are still misconceptions about nurses and injections.
“Only doctors can give injections”
This is not true. Nurses are fully trained and authorised to administer injections within their scope of practice.
“Injections are simple and require little training”
In reality, administering injections safely requires significant knowledge and skill.
“All nurses can give any type of injection”
Different types of injections require different levels of training. Nurses must be specifically trained and competent for each procedure.
The Importance of Patient Trust
Trust is a cornerstone of healthcare. Patients rely on nurses to provide safe, effective, and compassionate care. When it comes to injections, trust is particularly important, as many people feel anxious about needles.
Nurses play a key role in:
- Reassuring patients
- Explaining procedures clearly
- Minimising discomfort
- Responding to concerns
A skilled nurse can make the experience of receiving an injection far less stressful.
Future Trends in Nursing and Injections
Healthcare is constantly evolving, and the role of nurses continues to expand. Advances in technology, changes in healthcare delivery, and increased demand for services are shaping the future.
Trends include:
- Greater use of nurse prescribers
- Expansion of community-based care
- Increased focus on preventative healthcare, including vaccinations
- Development of new injection techniques and devices
As these trends continue, nurses will remain at the forefront of administering injections safely and effectively.
Why This Matters for Patients and Families
Understanding that nurses are qualified to give injections can provide reassurance and confidence. Whether receiving a vaccine, managing a chronic condition, or recovering from illness, patients can trust that trained nurses are equipped to deliver care safely.
For families and carers, this knowledge can also help in making informed decisions about healthcare services, particularly when considering home-based care.
So, are nurses allowed to give injections? Yes, they are not only allowed but are highly trained and trusted professionals who play a vital role in administering injections across a wide range of healthcare settings.
Their ability to perform this task is supported by rigorous training, strict regulations, and ongoing professional development. From hospitals to community clinics and home care environments, nurses ensure that injections are delivered safely, effectively, and with patient comfort in mind.
As healthcare continues to evolve, the role of nurses in administering injections will only become more important. For patients, this means greater access to high-quality care delivered by skilled and compassionate professionals.
How Nurses Ensure Best Practice When Giving Injections
Maintaining best practice is essential when administering injections. Nurses follow evidence-based guidelines to ensure that every procedure is carried out safely and consistently. This involves not only technical skill but also critical thinking and clinical judgement.
Before giving any injection, nurses conduct a thorough assessment. This may include reviewing the patient’s medical history, checking for allergies, and confirming the appropriateness of the medication. In many cases, especially in community care, nurses also evaluate the patient’s environment to ensure it is suitable for the procedure.
Documentation is another key aspect. Every injection must be recorded accurately, including the medication given, dosage, time, and any reactions observed. This creates a clear record that supports continuity of care and accountability.
The Importance of Infection Control
Infection prevention is a fundamental part of administering injections. Even a minor lapse in hygiene can lead to serious complications. Nurses are trained to follow strict infection control protocols, which include:
- Washing hands thoroughly before and after the procedure
- Using single-use, sterile needles and syringes
- Cleaning the injection site with an appropriate antiseptic
- Avoiding contamination of equipment
- Disposing of sharps immediately and safely
These measures are especially important in home care settings, where maintaining a clinical environment can be more challenging. Professional nurses are trained to adapt while still upholding the highest standards.
Managing Patient Anxiety and Pain
For many individuals, injections can be a source of anxiety or fear. Nurses are not only responsible for the technical aspect but also for the emotional wellbeing of the patient.
Effective strategies include:
- Explaining the procedure in simple, reassuring language
- Using distraction techniques
- Applying the correct injection technique to minimise discomfort
- Encouraging relaxation and steady breathing
Experienced nurses understand that a calm and confident approach can significantly improve the patient’s experience.
The Role of Consent and Communication
Consent is a legal and ethical requirement in all healthcare procedures, including injections. Nurses must ensure that patients understand:
- What the injection is for
- What the procedure involves
- Any potential risks or side effects
Patients have the right to ask questions and to refuse treatment. Nurses must respect these decisions while providing clear and accurate information.
Good communication also extends to working with other healthcare professionals. Nurses often collaborate with doctors, pharmacists, and carers to ensure that the patient receives coordinated and effective care.
Handling Adverse Reactions
Although most injections are routine, there is always a possibility of adverse reactions. Nurses are trained to recognise and respond to these situations promptly.
Reactions may include:
- Mild side effects such as redness or swelling at the injection site
- Allergic reactions
- Anaphylaxis, which is a severe and potentially life-threatening condition
In the event of a reaction, nurses follow emergency protocols, which may involve administering additional medication, monitoring vital signs, and seeking urgent medical support.
This level of preparedness is one of the reasons why trained nurses are trusted to carry out injections safely.
Injections and Medication Management
Administering injections is closely linked to medication management. Nurses must have a strong understanding of the medications they are giving, including:
- How the drug works
- The correct dosage
- Possible side effects
- Interactions with other medications
This knowledge ensures that injections are not only administered correctly but also contribute effectively to the patient’s treatment plan.
Medication errors can have serious consequences, which is why nurses follow strict checking procedures. This often includes double-checking with another healthcare professional when necessary.
The Growing Demand for Skilled Nursing Care
The demand for skilled nursing services, including injection administration, is increasing across the UK. Factors contributing to this trend include:
- An ageing population
- The rise in chronic health conditions
- Increased preference for home-based care
- Pressure on hospitals and clinics
As a result, more patients are seeking reliable and professional nursing care outside traditional healthcare settings.
Accessing qualified nurses through trusted providers such as https://www.nurseagnes.co.uk/ ensures that patients receive safe, regulated, and high-quality care in the comfort of their own homes.
Ethical Responsibilities of Nurses
Ethics play a significant role in nursing practice. When administering injections, nurses must adhere to principles such as:
- Respect for patient dignity
- Confidentiality
- Honesty and transparency
- Accountability for their actions
These principles guide every aspect of care and help build trust between nurses and patients.
For example, if a mistake occurs, a nurse is expected to report it immediately and take appropriate action. This commitment to ethical practice is essential for maintaining professional standards and patient safety.
How Technology is Shaping Injection Practices
Advancements in medical technology are influencing how injections are administered. New devices and techniques are designed to improve accuracy, reduce pain, and enhance safety.
Examples include:
- Pre-filled syringes that reduce the risk of dosage errors
- Needle-free injection systems
- Smart devices that track medication administration
Nurses must stay updated with these innovations through ongoing training and professional development. This ensures that patients benefit from the latest advancements in care.
Training Pathways for Nurses in the UK
For those considering a nursing career, understanding the training pathway can be helpful. To become a registered nurse in the UK, individuals must:
- Complete an approved nursing degree
- Register with the Nursing and Midwifery Council
- Undertake continuous professional development
During their education, student nurses receive hands-on training in clinical skills, including injections. This is supported by supervised practice in real healthcare settings.
After qualification, nurses can pursue additional training to specialise in areas that involve advanced injection techniques.
Supporting Self-Administration of Injections
In some cases, patients are taught to administer their own injections, such as insulin for diabetes. Nurses play a crucial role in educating and supporting these patients.
This includes:
- Demonstrating the correct technique
- Providing guidance on dosage and timing
- Advising on safe storage and disposal of equipment
- Monitoring progress and addressing concerns
Empowering patients in this way can improve independence and quality of life while reducing the need for frequent clinical visits.
Final Thoughts
The question “are nurses allowed to give injections” reflects a broader curiosity about the capabilities and responsibilities of nursing professionals. In reality, administering injections is a core part of nursing practice, supported by extensive training, strict regulation, and a commitment to patient safety.
Nurses are not only permitted to give injections but are often the primary professionals responsible for delivering them across a wide range of healthcare settings. Their expertise ensures that patients receive timely, effective, and compassionate care.
As healthcare continues to evolve, the role of nurses will remain essential. Whether in hospitals, clinics, or home environments, their ability to safely administer injections is a vital component of modern medical care.