Can you inject as a nurse?
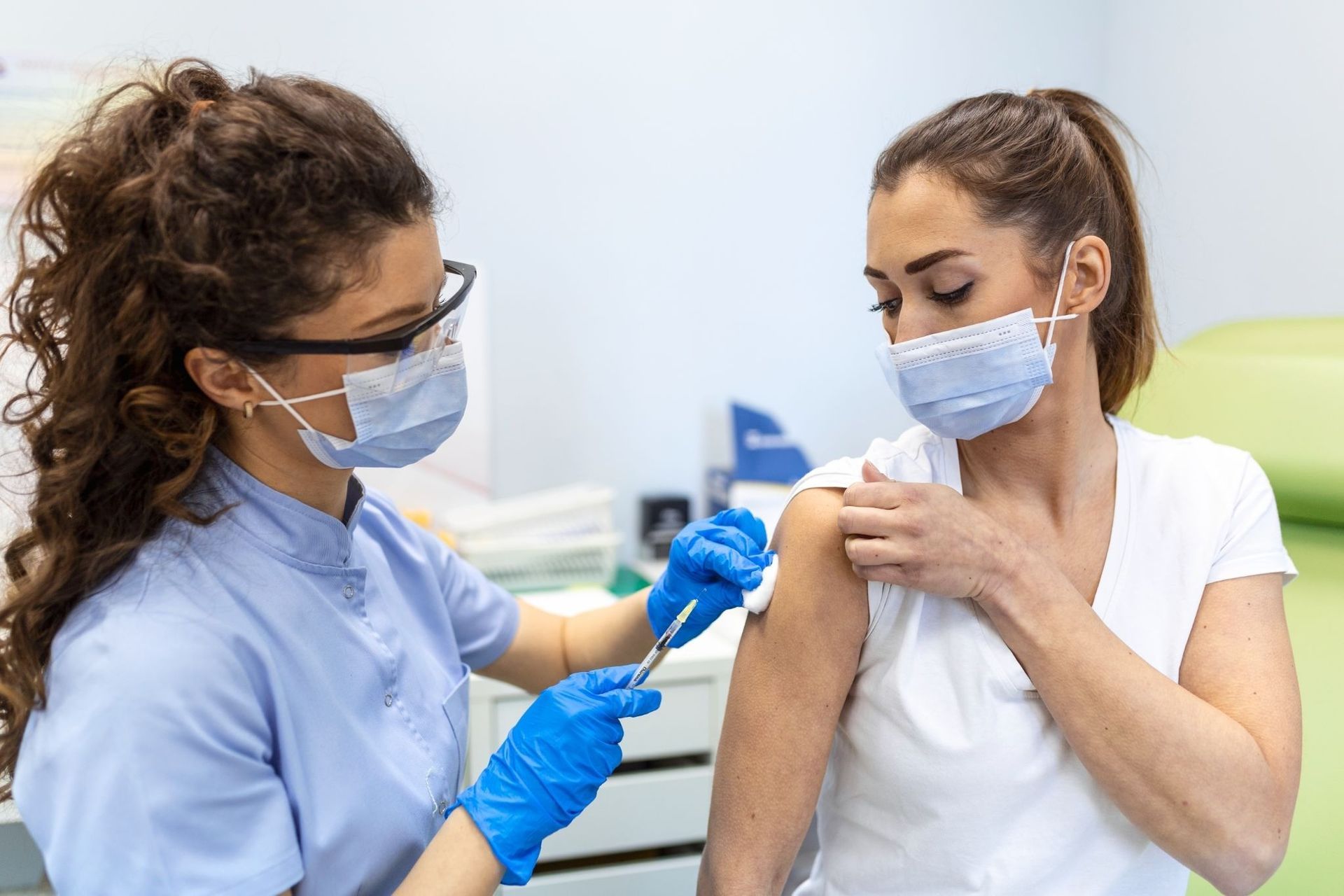
Administering injections is one of the most recognisable clinical skills associated with nursing. From vaccinations to life-saving medications, injections play a central role in modern healthcare delivery. However, a common question people search online is simple yet important: can you inject as a nurse? The answer is yes, but with clear conditions, training requirements, and professional responsibilities attached.
This guide explores everything you need to know about injection administration in nursing practice. It covers legal scope, types of injections, required competencies, training pathways, and patient safety considerations. Whether you are a student nurse, a qualified practitioner, or someone considering a healthcare career, this article provides authoritative and practical insights.
Understanding the Scope of Nursing Practice
In the United Kingdom, nurses are regulated professionals who must adhere to strict standards of care. Injection administration is not automatically granted upon qualification. Instead, it falls within a nurse’s scope of practice, which is defined by:
- Professional registration and training
- Clinical competence
- Employer policies
- Local protocols and guidelines
A registered nurse can administer injections only when they are trained, assessed as competent, and authorised by their workplace. This ensures patient safety and maintains high standards of care.
What Types of Injections Can Nurses Administer?
Nurses are trained to deliver a wide range of injections across different clinical settings. These include:
Intramuscular (IM) Injections
These are delivered into the muscle, often used for vaccines, antibiotics, and certain hormone treatments.
Subcutaneous (SC) Injections
Administered into the fatty tissue beneath the skin. Common examples include insulin and anticoagulants.
Intradermal (ID) Injections
Given just under the skin’s surface, typically used for allergy testing or tuberculosis screening.
Intravenous (IV) Injections
Delivered directly into a vein. This method requires advanced training and is often used in hospital settings for rapid medication administration.
Each type requires a different technique, anatomical knowledge, and level of expertise. Nurses must be competent in the specific method they are performing.
Do All Nurses Learn Injection Skills?
Yes, injection techniques are usually introduced during pre-registration nursing education. However, theoretical learning alone is not enough. Competency is achieved through:
- Supervised clinical practice
- Skills assessments
- Ongoing evaluation in real-world settings
Even after qualification, a nurse must not perform injections independently until they have demonstrated competence in their workplace.
Training and Competency Requirements
To administer injections safely and legally, nurses must complete structured training and competency assessments. This typically includes:
Theoretical Knowledge
Understanding pharmacology, dosage calculations, infection control, and anatomy.
Practical Training
Hands-on experience under supervision, including preparation, administration, and disposal of sharps.
Competency Sign-Off
Formal evaluation by a qualified assessor to confirm the nurse can perform injections safely.
Continuing Professional Development
Skills must be regularly updated to remain current with best practices and new treatments.
Specialised areas such as aesthetic nursing or travel health may require additional certifications.
Legal and Professional Responsibilities
Administering injections carries significant responsibility. Nurses must follow professional standards to ensure patient safety and legal compliance.
Key responsibilities include:
- Obtaining informed consent from the patient
- Checking the correct medication, dose, and route
- Maintaining aseptic technique
- Documenting the procedure accurately
- Monitoring for adverse reactions
Failure to follow these standards can lead to serious consequences, including professional misconduct investigations.
Can Student Nurses Give Injections?
Student nurses can administer injections, but only under direct supervision. They must:
- Be deemed competent for the specific procedure
- Work within their level of training
- Be supervised by a qualified nurse or mentor
This supervised experience is essential for developing confidence and competence before becoming fully registered.
Advanced Nursing Roles and Injection Authority
As nurses progress in their careers, they may take on advanced roles that expand their scope of practice.
Nurse Prescribers
Some nurses undertake additional training to become independent or supplementary prescribers. This allows them to prescribe and administer medications, including injections.
Specialist Nurses
Roles such as diabetes nurses, oncology nurses, and practice nurses often involve frequent injection administration as part of routine care.
Aesthetic Nurses
In private healthcare, nurses may train in cosmetic procedures such as dermal fillers and anti-wrinkle injections. These require specialist courses and adherence to strict regulatory frameworks.
Injection Safety and Best Practice
Safety is the cornerstone of injection administration. Nurses must follow evidence-based practices to minimise risk.
Infection Control
Using sterile equipment, proper hand hygiene, and safe disposal of sharps reduces infection risk.
Correct Technique
Choosing the right site, needle size, and angle ensures effective delivery and reduces complications.
Patient Assessment
Before administering an injection, nurses must assess allergies, medical history, and potential contraindications.
Monitoring and Aftercare
Patients should be observed for adverse reactions, especially with vaccines or new medications.
Common Risks and How Nurses Manage Them
Although injections are routine, they are not without risks. Nurses are trained to identify and manage potential complications such as:
- Injection site reactions
- Allergic responses
- Incorrect dosage or medication errors
- Needle-stick injuries
Risk management includes following protocols, double-checking medications, and using safety-engineered devices.
The Importance of Documentation
Accurate record-keeping is a legal and professional requirement. After administering an injection, nurses must document:
- Medication name and dose
- Route and site of administration
- Time and date
- Patient response
- Any adverse effects
Good documentation ensures continuity of care and protects both patient and practitioner.
Can Nurses Refuse to Give an Injection?
Yes, nurses have the professional right to refuse if:
- They are not trained or competent
- The prescription is unclear or unsafe
- The patient refuses consent
In such cases, the nurse must escalate the issue to a senior colleague or prescribing professional.
Career Opportunities Involving Injection Skills
Injection administration opens doors to a wide range of nursing roles, including:
- General practice nursing
- Community healthcare
- Occupational health
- Travel clinics
- Aesthetic medicine
These roles often require strong clinical skills, communication abilities, and ongoing professional development.
Why Proper Training Matters
Injection administration may seem straightforward, but it involves complex clinical judgement. Proper training ensures:
- Patient safety
- Effective treatment outcomes
- Compliance with legal standards
- Professional credibility
For those interested in expanding their clinical skills or entering specialist areas, high-quality training is essential. You can explore professional nursing support and guidance at https://www.nurseagnes.co.uk/.
Frequently Asked Questions
Can a newly qualified nurse give injections?
Yes, but only after being assessed as competent in their workplace.
Do nurses need a prescription to give injections?
In most cases, yes. Unless they are qualified prescribers, nurses administer medications prescribed by a doctor or authorised professional.
Are injections part of every nursing job?
Not necessarily. While common, some roles may involve minimal or no injection work.
Can nurses give cosmetic injections?
Yes, with additional specialised training and adherence to regulatory guidelines.
So, can you inject as a nurse? The answer is a clear yes, but it comes with responsibility, training, and professional accountability. Injection administration is a core nursing skill that requires precision, knowledge, and ongoing competence.
Whether working in hospitals, community settings, or specialised clinics, nurses play a vital role in delivering safe and effective injectable treatments. By maintaining high standards of practice and continuing professional development, nurses ensure they provide the best possible care to their patients.
If you are considering a career in nursing or looking to expand your clinical expertise, understanding injection practice is an essential step toward professional growth.
Building Confidence in Injection Administration
For many nurses, confidence in administering injections develops over time through repetition, mentorship, and reflective practice. While initial training provides the foundation, real competence is built in clinical environments where nurses encounter diverse patient needs.
Confidence comes from:
- Repeated supervised practice
- Constructive feedback from senior staff
- Understanding patient variability
- Learning from both routine and complex cases
It is important to recognise that hesitation is normal in the early stages. Safe practice always takes priority over speed, and asking for support is a sign of professionalism, not weakness.
Communication Skills and Patient Experience
Administering an injection is not just a technical procedure. It is also a patient interaction that can influence trust and overall care experience. Many patients feel anxious about needles, and nurses play a key role in easing that anxiety.
Effective communication includes:
- Explaining the purpose of the injection clearly
- Reassuring the patient about the procedure
- Gaining informed consent
- Using calm and confident language
- Observing non-verbal cues such as fear or discomfort
A nurse who communicates well can significantly reduce patient distress and improve cooperation during the procedure.
Ethical Considerations in Injection Practice
Nurses must always act in the best interests of their patients. Ethical practice is central to injection administration and includes respecting patient autonomy and dignity.
Key ethical principles include:
Consent
Patients have the right to accept or refuse treatment. Consent must be informed, voluntary, and documented when required.
Confidentiality
All patient information related to treatment must be kept secure and shared only with relevant healthcare professionals.
Non-maleficence
Nurses must avoid causing harm by ensuring correct procedures and safe medication practices.
Beneficence
Every injection should be given with the intention of benefiting the patient’s health and wellbeing.
Infection Prevention and Control in Detail
Infection control is one of the most critical aspects of injection administration. Poor technique can lead to serious complications, including local infections and systemic illness.
Best practices include:
- Performing hand hygiene before and after each procedure
- Using single-use sterile needles and syringes
- Cleaning the injection site with appropriate antiseptic
- Avoiding re-use of equipment under any circumstances
- Disposing of sharps immediately in approved containers
Healthcare settings in the UK follow strict infection control guidelines, and nurses are expected to comply at all times.
Sharps Safety and Needle Disposal
Handling needles safely is essential to prevent injuries and cross-contamination. Needle-stick injuries can expose healthcare workers to blood-borne infections, making prevention a top priority.
Important safety measures include:
- Never recapping needles after use
- Using safety-engineered devices where available
- Disposing of needles immediately after use
- Reporting any needle-stick injury promptly
- Following post-exposure protocols if an incident occurs
Employers are legally required to provide appropriate training and equipment to reduce these risks.
Cultural Sensitivity and Patient-Centred Care
In a diverse healthcare environment, nurses must be aware of cultural, religious, and personal beliefs that may influence a patient’s response to injections.
Examples include:
- Patients who prefer same-gender healthcare providers
- Cultural beliefs about certain medications
- Religious considerations related to vaccines or treatments
Providing patient-centred care means respecting these preferences wherever possible while ensuring safe and effective treatment.
Technology and Innovation in Injection Practice
Healthcare is constantly evolving, and injection practices are no exception. New technologies are improving both safety and patient comfort.
Some innovations include:
- Needle-free injection systems
- Smart syringes with safety locks
- Pre-filled medication devices
- Digital documentation systems
Nurses must stay updated with these advancements as part of their continuing professional development.
Challenges Nurses Face When Administering Injections
Despite being a routine task, injection administration can present challenges such as:
- Managing anxious or uncooperative patients
- Working under time pressure in busy clinical settings
- Dealing with complex medication regimens
- Ensuring accuracy in high-risk environments
Overcoming these challenges requires strong clinical judgement, time management, and teamwork.
The Role of Policies and Guidelines
Every healthcare organisation in the UK has policies that govern injection administration. These are based on national standards and evidence-based practice.
Nurses must:
- Follow local protocols at all times
- Stay updated with changes in guidelines
- Participate in regular training sessions
- Report any deviations or incidents
Adhering to these policies ensures consistency, safety, and legal compliance across healthcare settings.
Expanding Your Skills as a Nurse
Injection administration can be a gateway to advanced clinical skills. Nurses who wish to specialise can pursue additional training in areas such as:
- Vaccination programmes
- Chronic disease management
- Travel medicine
- Cosmetic procedures
- Emergency care
Developing expertise in these areas can enhance career prospects and increase professional satisfaction.
Real-World Application in Different Settings
Injection practices vary depending on the clinical environment. Understanding these differences helps nurses adapt their skills effectively.
Hospitals
Nurses often administer IV medications, manage complex drug regimens, and respond to acute patient needs.
GP Surgeries
Practice nurses frequently give vaccinations, hormone injections, and routine medications.
Community Care
Nurses may visit patients at home to administer injections, requiring strong independence and adaptability.
Private Clinics
Specialist services such as aesthetics or travel health involve tailored injection techniques and patient education.
How Patients Can Feel More Comfortable
Patients often search for reassurance about injections. Nurses can help by:
- Using distraction techniques
- Applying gentle and efficient techniques
- Offering clear explanations
- Encouraging relaxation methods
A positive experience can reduce fear in future healthcare interactions.
Why This Topic Matters for Healthcare Awareness
The question “can you inject as a nurse” reflects a broader public interest in understanding healthcare roles.
Clear, accurate information helps:
- Build trust in healthcare professionals
- Educate patients about safe practices
- Encourage informed decision-making
- Support those considering a nursing career
Providing reliable answers also strengthens online visibility for healthcare platforms and educational resources.
Conclusion
Injection administration is a fundamental yet highly skilled aspect of nursing practice. While the answer to whether nurses can give injections is yes, it is supported by rigorous training, legal frameworks, and ongoing professional development.
From ensuring patient safety to maintaining ethical standards, nurses carry significant responsibility when performing this task. With the right training and commitment to best practice, injection administration becomes a safe, effective, and rewarding part of patient care.
For those seeking professional insight, training guidance, or support in nursing practice, visiting
https://www.nurseagnes.co.uk/ can provide valuable resources and expert information tailored to modern healthcare needs.